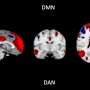
Researchers from Université Savoie Mont Blanc, Radboud University, and the University of Oxford’s Wellcome Center for Integrative Neuroimaging have identified a potential fMRI biomarker linked to cognitive decline in Alzheimer’s disease. Their study, published in NeuroImage, highlights the attenuation of intrinsic anticorrelation between the brain’s default mode network (DMN) and dorsal attention network (DAN) as a significant indicator of Alzheimer’s pathology that is somewhat independent of tau pathology and educational background.
Alzheimer’s disease continues to challenge researchers, who have yet to find a single reliable biomarker to determine when and where abnormal protein accumulation leads to cognitive decline and irreversible brain damage. Current understanding of the large-scale functional breakdown in the disease remains incomplete. It involves complex interactions between amyloid and tau pathologies, vascular lesions, and neurodegeneration. As beta-amyloid accumulation begins years before clinical symptoms appear, it supports the notion of Alzheimer’s as a continuum, urging researchers to explore beyond mere protein accumulation for insights.
Understanding Brain Networks
The human brain’s neurocognitive networks can exhibit cooperation or competition. Using resting-state functional MRI, researchers have studied interactions among these networks without the necessity of performing tasks. The DMN and DAN are two large-scale systems that typically exhibit an on/off relationship. When the DMN is active—associated with daydreaming or self-reflection—the DAN is inactive, and vice versa.
Past studies have shown that resting-state functional connectivity within and between large networks correlates with cognitive performance in healthy adults. Alzheimer’s disease disrupts these connectivity patterns, leading to cognitive decline. A concept of “functional imbalance” in resting-state networks has emerged, suggesting that alterations could indicate neurodegenerative pathology. Therefore, the relationship between DMN-DAN connectivity, cognitive reserve, and pathology burden is of considerable interest.
In their study, researchers analyzed MRI and PET amyloid and tau imaging alongside cognitive assessments from 182 participants in the Alzheimer’s Disease Neuroimaging Initiative (ADNI) cohort. The objective was to investigate whether DMN-DAN anticorrelation associated with Alzheimer’s pathology burden and whether it represented a mechanism independent of tau-driven spread.
Key Findings and Implications
The findings revealed a reduced separation between DMN and DAN activity in participants with high amyloid burden and cognitive impairment. This diminished separation indicates that as networks become less distinct, cognitive processes become more susceptible to interference, complicating focus, information retrieval, and task coordination. In the complete cohort, a weaker DMN-DAN anticorrelation correlated with lower cognitive scores.
Multivariate models that included factors such as age, sex, education, and tau burden indicated that DMN-DAN connectivity acted as an independent predictor of cognitive performance, accounting for approximately 5% of the variance. This relationship extended to Mini-Mental State Examination scores and various tests from the ADNI neuropsychological battery, linking DMN-DAN anticorrelation to cognitive performance across numerous domains.
Interestingly, education level, often used to gauge cognitive reserve, did not alter this association, suggesting that the interplay between these networks is significant regardless of educational background.
The authors argue that these findings place a simple resting-state measure at the center of a complex narrative surrounding Alzheimer’s disease. They highlight that the separation of networks, which typically helps distinguish between internal and external focus, was least intact in participants who were amyloid positive and cognitively impaired. Rather than indicating a linear cascade from one structure to another, the research suggests a multifocal pattern of “strikes” across various cerebral and extracerebral systems—including vascular disease, sleep loss, and stress—that converge on a clinical syndrome.
This new perspective challenges previous interpretations that primarily viewed DMN-DAN changes as intermediaries of tau-dependent neurodegeneration. Instead, network behavior appears to serve as a candidate signal that accompanies pathology without being wholly explained by advanced tau accumulation or cognitive reserve.
Future research directions mentioned in the study include longitudinal and interventional studies to clarify whether network dysfunction precedes or follows abnormal protein accumulation. The authors also advocate for developing personalized risk models that incorporate normative DMN-DAN connectivity patterns, pathology measures, and lifestyle factors across extensive longitudinal datasets.
This research underscores the importance of exploring new avenues in Alzheimer’s studies, focusing on network functionality as a potential avenue for understanding cognitive decline.